By Emily Yan | Keysight Technologies
Electronic Medical Record (EMR) systems have taken center stage in developed nations, revolutionizing patient record management and streamlining treatment. With EMRs at the heart of healthcare infrastructure, they play a pivotal role in navigating patients through diverse medical interventions, encompassing primary, secondary, and even tertiary specialist care. These systems also grapple with the complexity and sensitivity of managing and sharing patient data, diligently governed by stringent regulations such as HIPAA to ensure the security of PHI. The insights gleaned from the Vital Signs survey by the Healthcare Information and Management Systems Society (HIMSS) shed light on some concerning issues regarding software testing in healthcare systems.
The Changing Role of EMR Systems
As the paradigm shifts towards a more data-centric approach in healthcare, the overall patient experience is gaining prominence. Given EMRs’ crucial role in providing accurate, readily accessible medical histories, any inaccuracies, omissions, or system failures can have severe implications for patient safety and outcomes. As of 2021, driven by HITECH and other government initiatives, nearly 80% of office-based physicians in the U.S. have adopted certified EMR systems. However, a significant finding of the 2020 U.S. study indicated that EMR systems failed to detect up to 33% of drug interactions and medication errors, revealing potential threats to patient safety.
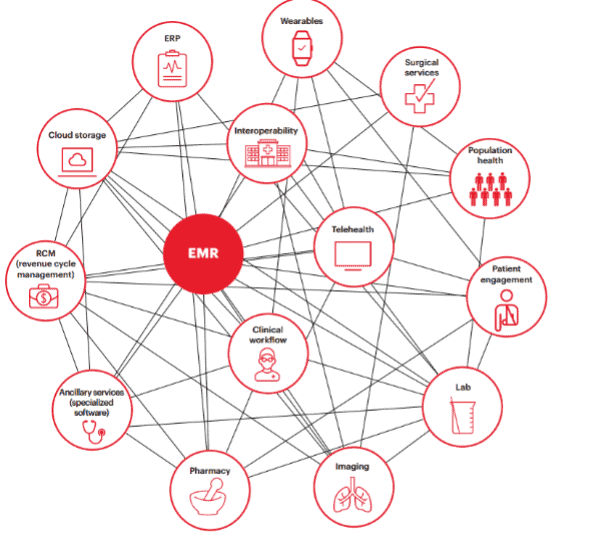
Figure 1. EMR’s central role in the ever-growing digital healthcare landscape
The presence of erroneous EMR data brings about numerous pitfalls, posing risks to patient safety and leading to inefficiencies and delays in workflow. These issues arise from application misconfiguration and poorly designed user interfaces. This scenario only amplifies patient anxiety and frustration, underscoring the indispensable need for thorough EMR testing across functionality, performance, integration, and usability.
Furthermore, the absence of interoperability among various EMR/EHR platforms compels hospitals to juggle multiple systems, often dealing with at least 10 platforms in most cases. The need to manage and update multiple platforms incurs costs that can easily outrun manual testing teams’ capacity.
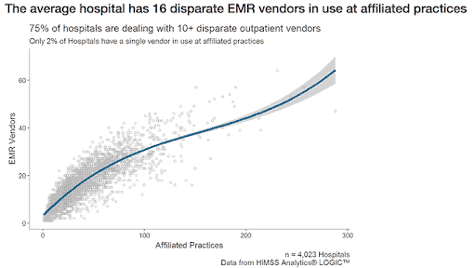
Figure 2. Average hospitals have 16 disparate EMR vendors in use (Source: Healthcare IT News)
Key Challenges in EMR Quality Assurance
Despite the rapid advancements and rising complexity of new EMR developments and integration requirements, the HIMSS survey reveals a stark reality: only 15% of healthcare providers surveyed adopted test automation platforms.
Traditional manual testing methods, unfortunately, do not scale to meet the increasing and complex demands of testing, leading to:
- Merely 33% of manual testers are satisfied with their organizations’ capacity to scale testing to meet new requirements.
- Only 38% are satisfied with the availability of clear testing analytics.
- Only 38% of manual testers believe their organizations can adequately develop test coverage across all devices and browsers.
DIY Testing Mistakes to Avoid
The DIY testing approach, preferred by over 40% of respondents, has drawbacks that make it counterproductive and inefficient. Challenges include a lack of technical talent, hidden costs, potential release delays, and difficulties in achieving comprehensive test coverage.
A recent Forrester report reveals that 63% of organizations adopting a DIY approach rely on three or more development tools or automation solutions for testing. This underscores the complexity of healthcare applications and the need for specialized expertise in diverse automation frameworks and programming languages. As a result, only 38% of respondents in the HIMSS study utilizing DIY testing methods express satisfaction with their organization’s ability to enhance the job satisfaction and productivity of their QA teams. This satisfaction rate is five percentage points lower compared to teams that rely on manual testing approaches.
AI to the Rescue
However, there is a silver lining: projections indicate that 75% of healthcare providers plan to adopt automated testing within the next five years. Early adopters are already reaping the benefits, with 80% expressing satisfaction with their organization’s ability to scale testing to meet emerging requirements.
With the dawn of AI and machine learning in healthcare software testing, next-gen test automation platforms enable automatically generating maximum test coverage and accuracy. For instance, AI can create a digital twin model for functional, regression, and user experience testing across any device, platform, or operating system – testing the EMR software as a clinician would. This typically includes automating all major aspects of testing, from low-level test execution all the way up to high-level test design. In addition, AI can analyze real-time data and provide predictive metrics on release quality.
A Path Forward
In the end, it is important to remember that testing is not merely an end in itself, but a critical component in delivering tangible business value. In healthcare, this translates into enhanced patient outcomes, increased safety, and improved patient experiences.
To deepen your understanding of the key trends and challenges in healthcare software testing, I recommend reviewing the comprehensive findings of the Vital Signs study or the short summary. The insights therein can be instrumental in bolstering your future testing strategies and thereby contribute to safeguarding patient lives.
This is a contributed guest post
Digital Health Buzz!
Digital Health Buzz! aims to be the destination of choice when it comes to what’s happening in the digital health world. We are not about news and views, but informative articles and thoughts to apply in your business.