The average waiting time for an MRI scan is 21 days, according to the latest Diagnostic Imaging Dataset published by NHS England.
This compares to same day for X-Rays, Fluoroscopy and Medical Photography.
Yet even that 21 day figure, extracted by NHS Digital from local Radiology Information Systems, masks the true extent of the problem.
It’s skewed by the number of in-patients who have their test done far quicker.
A third (33%) of the two million out-patients referred for an MRI scan in England have to wait over a month – with a further 10% waiting two months or more.
And the actual total wait could be five months or even longer.
This is because the NHS Digital figures only show the time between the MRI scan being requested and the date of the test. It doesn’t take into account the time it takes to be referred for the scan in the first place.
Just 16% of out-patients are scanned within a week, compared with 93% of people already in hospital.
But it’s not just delay that is a problem with the imaging technology provided by the NHS.
Our research suggests that nearly a third of people in the UK suffer from claustrophobia at some point in their lives. This fear of small spaces seems to be worse for women, affecting 36%, compared to 27% of men.
Avoiding situations known to trigger attacks is the most common step taken to help, whilst others rely on breathing techniques or focus on relaxing images.
A ‘tunnel’ MRI scanner is one of the three worst scenarios for claustrophobia, along with crowded places and a tiny room with no windows.
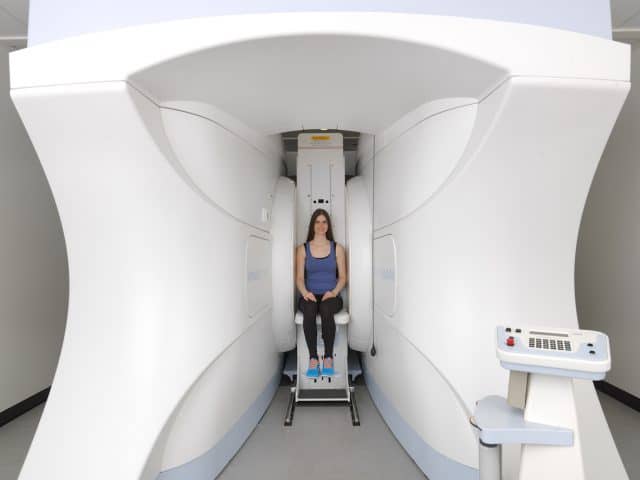
Over half of those who’ve been scanned in an enclosed MRI tube said they felt very nervous. A further 10% required sedation and another 13% asked for the process to be stopped altogether.
Yet only 5% of patients have been offered an upright open MRI scan by their referring physician.
Everyone else is required to slide into a tight, cramped, noisy tunnel – the top of which is just centimetres from your face. Many people find this experience terrifying – inducing panic attacks and increases in blood pressure.
At Medserena we estimate that nearly half a million MRI scans are disrupted every year as a result of claustrophobia. Disrupted meaning re-scheduled, aborted during the process, delayed due to a request for sedation or cancelled altogether. That represents wasted time, slots that could be available to other patients and, of course, it’s a huge burden on the strapped NHS budget.
Why, therefore, does the NHS not offer upright, open scans to more patients?
One of the reasons is that many doctors and consultants simply don’t know that the option exists.
We are finding that, increasingly, the initiative is being taken by patients themselves having done a quick bit of research on the internet.
They realise that instead of being crammed into a narrow tunnel they can sit or stand in an entirely open scanner – and actually watch TV on a large 50” screen whilst the examination is in progress! So they demand a referral for an upright, open MRI.
Even the head coils for brain scans are designed to allow a clear view of the surrounding area outside the system at all times – and a friend or relative is welcome to stay with them in the room.
But there are other, clinical justifications for using upright positional MRI rather than the conventional tunnel. It can provide medical benefits not duplicated by other MRI technology, especially in the evaluation of spinal pathology. Mermaid Beach Radiology for instance can provide you with MRI services.
One key feature of upright MRI is that scans are carried out in a natural weight-bearing position. In many cases, this provides a more conclusive diagnosis than supine MRIs for symptoms such as back pain.
The intervertebral discs are exposed to a pressure that is 11 times greater when sitting, and 8 times greater when standing, than when recumbent. These load-dependent changes can reveal pathology that is at worst not visible, or at best underestimated, in a tunnel situation.
Upright Open MRIs allow almost complete freedom of movement. For instance, in addition to standing or sitting upright, the spinal column can be imaged with flexion (bending forwards), extension (stretching backwards), rotation and even lateral bending to the point where pain is at its most acute.
It simply isn’t possible to perform flexion and extension scans of the cervical spine or neck (Cranio-cervical junction) when supine!
So the real advantage is that the weight-bearing structures of the body can be imaged under physiological loading.
We can now capture images and clearly prove instabilities as a result of vertebral slipping or position-dependent disc herniation, leading to a more accurate diagnosis.
Indeed, we’ve seen many cases of people who’ve had digital scans previously that didn’t detect any abnormalities, whereas we’ve been able to identify the root cause. Reaching the correct diagnosis quickly is naturally of paramount importance to the patient
Most worryingly, our research showed that a quarter of people with claustrophobia said they would prefer to leave a medical condition untreated, if they were very frightened of the test to diagnose it. Even if they were experiencing pain on a daily basis.
So patients can literally get sent home with no diagnostic imaging performed.
21st Century medical device technology really has to be better than that!
If you, a relative or friend have been referred for an MRI scan but feel that a weight-bearing scan would be more beneficial or don’t like the idea of a conventional tunnel MRI, advice and information is available at: https://www.trulyopenmri.com/
This article was sponsored by Starfish PR
Professor Francis Smith, Clinical Director at Medserena Upright Open MRI Centre
Professor Francis Smith pioneered the clinical application of MRI, starting the world’s first clinical trial in 1980 and the first diagnostic MRI service at Aberdeen Royal Infirmary in 1981. He worked in collaboration with a number of clinicians exploring the applications of MRI, being the first to show its potential in the examination of the abdomen and pelvis as well as for the study of pregnancy. He published the first clinical applications of MRI to musculoskeletal radiology, head and neck malignancy, liver and pancreatic disease, pelvic malignancy and pregnancy. He has over 250 publications in peer reviewed Journals, 32 book chapters and has co-authored 5 text books. He is currently Consultant Radiologist and Clinical Director at the Medserena Upright Open MRI centres in London and Manchester.